EQUITABLE ACCESS TO HEALTH CARE SERVICES FOR ALL BRITISH COLUMBIANS (2025)
Issue
The current funding model for healthcare infrastructure in Canada is intended to provide equitable access to necessary medical services for ALL Canadians. Currently, there are several regions of British Columbia that lack adequate medical infrastructure to deliver even the most necessary medical services to the populations they are serving.
To ensure that all British Columbians have equitable access to necessary medical services, the Province must negotiate new 2026-2028 bilateral agreements with the Federal government that include the provision of tertiary care medical services for our rural and vulnerable populations on Vancouver Island, Northern BC and Interior Health regions.
Background
The majority of Canada’s current hospital stock was financed through a National Health Grants program from 1948 through 1971. The federal health grants provided matching funds to provincial government grants to build community hospitals. It is estimated that 90% of Canada’s hospitals were created over the course of this program.[1]
The Canada Health Act is a federal law establishing the framework for the publicly funded healthcare system. Every province and territory in Canada must ensure that its health care insurance plans meet the standards of the Canada Health Act. The standards described in the Act include accessibility, portability, universality, comprehensiveness and public administration.[2]
The primary objective of Canada’s health care policy is to “protect, promote, and restore the physical and mental well-being of residents of Canada and to facilitate reasonable access to health services without financial or other barriers”.[3]
Under the Canada Health Act, there are criteria and conditions related to insured health services and extended health care services that the provinces and territories must fulfill to receive the full federal cash contribution under the Canada Health Transfer.[4] British Columbia is not meeting these criteria in several regions in the Province.
The underlying goal of the Canada’s health service policy is not to levy penalties, but to ensure access to medically necessary care. British Columbia ranks second-last in healthcare access across Canada. A study show 24% of British Columbians struggle with consistent issues in gaining necessary medical services.[5]
Currently, tertiary care facilities in British Columbia are only found in Vancouver, Surrey, Victoria, Kelowna and Kamloops. Even relatively large cities in British Columbia do not have direct access to tertiary care, such as Nanaimo, Penticton and Prince George. Accessing tertiary care services in our northern and rural communities in British Columbia remains a significant and critical challenge.[6]
In 2023, the Prime Minister and Premiers agreed on shared health priorities to deliver real results to Canadians, supported by additional federal health investments of close to $200 billion over 10 years to address gaps and improve integrated health care services under the ‘Working Together to Improve Health Care for Canadians Plan’. Through this plan, the Federal government aims to:[7]
- expand access to family health services, including rural and remote areas;
- support health workers and reduce backlogs for health services such as surgeries and diagnostics;
- improve access to quality mental health, substance use and addiction services;
- modernize the health care system with standardized information and digital tools so health care providers and patients have access to electronic health information;
- work with provinces and territories to help people in Canada age with dignity, closer to home by supporting efforts to improve access to home and community care and safe long-term care; and
- address unique challenges that Indigenous Peoples face when it comes to fair and equitable access to quality and culturally safe health services.
Funding from the plan is delivered through bilateral agreements between the provinces and territories and the Federal government.
In 2023, Ontario, with a population of approximately 16 million people, negotiated a bilateral agreement to receive $73.97 billion in funding over 10 years under the plan.
By comparison, BC, with a population of approximately 5.6 million people, negotiated a bilateral agreement to receive $7.5 billion in funding over 3 years.[8] Based on population, BC’s fair share of the total federal funding available over the next 10 years is approximately $25 billion.
The Working Together to Improve Health Care for Canadians Plan emphasized the importance of upholding the Canada Health Act to protect Canada’s publicly funded health care system. A key aspect in upholding these principles is to ensure that Canadians do not face charges for medically necessary care, and that when innovations are introduced into our health care system, it is important to ensure that they benefit all Canadians equally.[9]
In 2023, 104 of Canada’s 1017 hospital establishments were located in British Columbia, representing approximately 10% of the Canada’s healthcare infrastructure. Based on population, British Columbia’s share of the federal health investments promised over the next 10 years is approximately $25 billion.
The Lower Mainland and Southern Vancouver Island hospitals are seeing their share of these federal health investments. For example, the new Surrey hospital project saw its first major concrete pour in December 2024 after receiving $2.88 billion in government funding from the Province. The project is expected to employ up to 5000 trades over the 5 year construction period and create thousands more indirect jobs. Once complete approximately 2000 workers will be employed at the hospital. The project was made possible with community support and a 10 year capital plan.[10] The current population of Surrey is approximately 680,000.
Vancouver Island as a Business Case
The population on Vancouver Island is one of the fastest growing and fastest aging in Canada. 460,000 people are living North of the Malahat versus 445,000 people who live on the Southern portion of Vancouver Island. By comparison, the Northern Health authority serves a population of approximately 300,000 people and has the least access to equitable medical services.
The Central Island has the oldest population in Canada driving high acute care demands. In addition, 80% of the Island’s First Nations are in the Nanaimo Regional General Hospital (NRGH) catchment area. Currently patients in this area do not have access to equitable care they need and have a right to and many suffer poorer outcomes that are sometimes fatal.
Victoria has two catheterization labs whereas Nanaimo and Central/North Island have none making the North Island region the largest population over 400,000 in Canada without equitable access to this essential health care service. Additional statistics below show the gross disparity in equitable access to health care in the region showing that the Northern half of the Island’s population receives 1/5 of the health resources[11].
Table 1
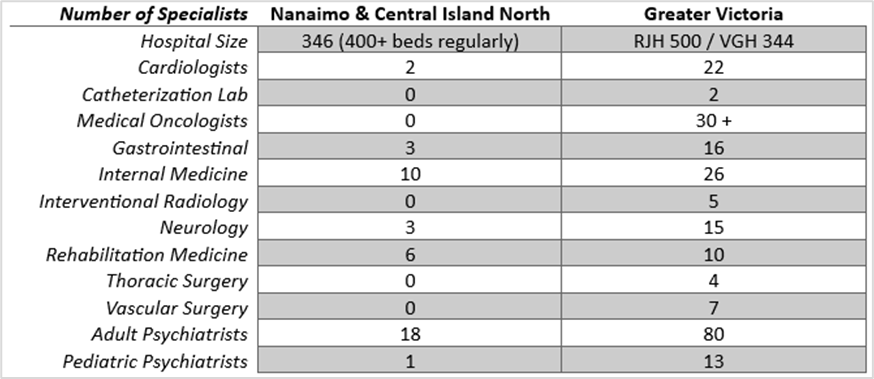
Our health care system in British Columbia is woefully under-resourced and has fallen far behind the growing needs of an expanding population. The Province is mandating housing start numbers and housing types for municipalities, but it is not supporting regional infrastructure and social supports that match the population growth it is promoting.
THE CHAMBER RECOMMENDS
That the Provincial Government:
- Allocate equitable health care funding from the 2025 bilateral agreement and a 5% annual top-up from the Federal government to underserved and underfunded regional health authorities in British Columbia.
- Negotiate British Columbia’s fair share of the Working Together to Improve Health Care of Canadians funding in the 2026-2028 bilateral agreements with the Federal government and commit to raising the basic standard of care in BC’s rural and vulnerable communities to meet the national minimum.
- Commit to expanding tertiary care level facilities in each regional health authority to meet the Canadian Standard of Care for 80% of the population of every health authority.
- Provide dedicated funding for health care facilities and emergency service providers to ensure that emergency rooms remain operational and first responders are available 24/7/365 in every rural community within the province.
[3] https://www.canada.ca/en/health-canada/services/health-care-system/canada-health-care-system-medicare/canada-health-act.htm
[4] https://www.canada.ca/en/health-canada/services/health-care-system/canada-health-care-system-medicare/canada-health-act.html
[5] Karamali & Sheffrey (2022, October 7) “British Columbians report 2nd worst access to health care in Canada” Global News
[7] https://www.canada.ca/en/health-canada/corporate/transparency/health-agreements/shared-health-priorities.html
[8] https://www2.gov.bc.ca/assets/gov/british-columbians-our-governments/organizational-structure/office-of-the-premier/bc-agreement-to-improve-health-care.pdf
[9] https://www.canada.ca/en/health-canada/services/health-care-system/canada-health-care-system-medicare/canada-health-act/letter-provinces-territories-january-2025.html
